Fentanyl has become the deadliest drug in the United States. The CDC has reported tens of thousands of overdose deaths linked to synthetic opioids each year, with fentanyl driving the majority of those losses. Its extreme potency — roughly 50 times stronger than heroin and 100 times stronger than morphine — makes it uniquely dangerous, and its presence in the illicit drug supply means that people using heroin, cocaine, methamphetamine, or counterfeit prescription pills may be exposed without knowing it.
If you or a loved one is struggling with fentanyl use, treatment is available and it works. Fentanyl addiction treatment in NY offers a path forward through evidence-based approaches that address both the physical grip of opioid dependence and the mental health challenges that often accompany it.
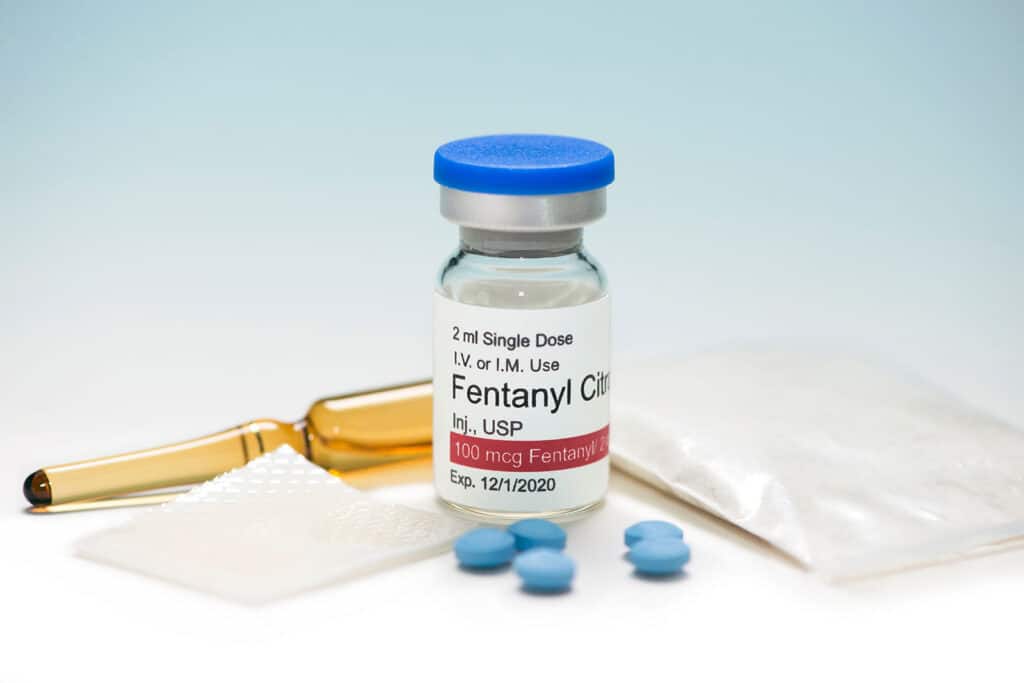
Understanding Fentanyl and Why It Is So Dangerous
Fentanyl is a synthetic opioid originally developed for medical use. Doctors have prescribed it for decades to manage severe pain, including during surgical procedures, for cancer patients, and in epidural form during childbirth. Pharmaceutical fentanyl is available as transdermal patches, lozenges, and injectable formulations.
The crisis stems from illicitly manufactured fentanyl, which has flooded the drug supply since around 2014. Because fentanyl is lethal at doses as small as two milligrams — a quantity barely visible to the naked eye — the margin between a dose that produces a high and one that causes fatal respiratory depression is extremely thin. Drug dealers cut fentanyl into heroin, cocaine, methamphetamine, and pressed counterfeit pills to increase potency and stretch their supply. This practice is responsible for a staggering number of overdose deaths, as users often have no idea what they are actually consuming.
Recognizing the Signs of Opioid Addiction
Fentanyl addiction, clinically referred to as opioid use disorder, can develop rapidly due to the drug’s potency. Common signs include an inability to control use despite negative consequences, needing increasing amounts to achieve the same effect (tolerance), spending significant time obtaining or using the drug, withdrawing from relationships and responsibilities, and experiencing withdrawal symptoms when not using. Recognizing these signs early and seeking professional assessment is an important first step toward recovery.

Treatment Options for Fentanyl Addiction
Effective fentanyl addiction treatment combines medications for opioid use disorder (MOUD) with behavioral therapy and supportive services. This integrated, evidence-based approach addresses the biological, psychological, and social dimensions of addiction.
Medications for Opioid Use Disorder (MOUD)
Medication-assisted treatment is the clinical standard for fentanyl addiction and has been shown to reduce overdose death, decrease illicit opioid use, and improve health and social function. The three primary medications used are:
Methadone is a long-acting opioid agonist administered through federally regulated opioid treatment programs. Methadone maintenance treatment works by occupying opioid receptors in the brain, preventing withdrawal symptoms and reducing cravings without producing the intense high associated with fentanyl. Treatment typically involves a daily dosing regimen at a clinic, though patients who demonstrate stability may earn take-home medication at increasing take-home levels over time.
Buprenorphine (Subutex) is a partial opioid agonist that can be prescribed in a doctor’s office, making it more accessible than methadone for many patients. Buprenorphine provides craving relief and withdrawal symptom prevention while carrying a lower risk of misuse due to its ceiling effect. It is available in sublingual tablets, films, and extended-release injectable formulations.
Suboxone (buprenorphine + naloxone) combines buprenorphine with naloxone, an opioid antagonist medication. The naloxone component discourages misuse by injection, as it triggers withdrawal if the medication is tampered with and injected rather than taken as directed. Suboxone is one of the most widely prescribed FDA-approved medications for opioid use disorder and can be initiated in outpatient settings, including via telehealth appointment in many cases.
Naltrexone (Vivitrol or Revia) is an opioid antagonist medication that blocks the effects of opioids entirely. Unlike methadone and buprenorphine, naltrexone is not a controlled substance and does not carry a risk of physical dependence. It is available as a daily oral tablet (Revia) or a monthly extended-release injection (Vivitrol). Naltrexone requires that the patient be fully detoxified from opioids before starting, which can be a barrier, but it is an effective option for people committed to long-term recovery who prefer a non-opioid treatment path.
Your treatment team will evaluate your history, the severity of your opioid use disorder, and any interactions with other medications or substances to determine which medication and treatment plan is the best fit.
Behavioral Therapy
Medication alone is rarely sufficient. Therapy sessions are a core component of comprehensive fentanyl addiction treatment. Common evidence-based approaches include:
Cognitive Behavioral Therapy (CBT) helps individuals identify and change the thought patterns and behaviors that drive substance use. It builds practical skills for managing triggers, stress, and high-risk situations.
Contingency Management provides tangible incentives for maintaining sobriety, such as vouchers or small rewards tied to clean drug tests, reinforcing positive behavior change.
Motivational Interviewing is a collaborative approach that strengthens an individual’s own motivation and commitment to change, which is particularly valuable in the early stages of recovery.
Family therapy sessions involve loved ones in the treatment process, addressing relationship dynamics, improving communication, and educating the support system about addiction and recovery. Family, friend, and support system education helps the people closest to the individual understand opioid use disorder and play a constructive role in the recovery process.
Holistic and Complementary Approaches
Many treatment programs now offer a holistic treatment experience that goes beyond medication and traditional talk therapy. These may include mindfulness and meditation, yoga, art and music therapy, exercise programming, nutrition counseling, and nonopioid therapies for pain management such as acupuncture or physical therapy. A whole-person approach addresses the underlying factors that contribute to addiction and supports sustained recovery.

Levels of Care: Finding the Right Fit
Fentanyl addiction treatment is not one-size-fits-all. The appropriate level of care depends on the severity of the addiction, co-occurring mental health conditions, the individual’s living situation, and their support network. A thorough assessment at intake helps determine the right starting point.
Medical Detoxification
Treatment typically begins with medically supervised detoxification. Fentanyl withdrawal symptoms can be severe and include muscle and bone pain, insomnia, diarrhea, vomiting, cold flashes, uncontrollable leg movements, intense cravings, anxiety, irritability, and attention problems. Long-term detoxification treatment in a medical setting ensures safety and comfort, with clinicians managing symptoms through appropriate medications.
Attempting to quit fentanyl without medical supervision is not only extremely uncomfortable but can be dangerous. Professional detox provides 24-hour monitoring and immediate access to care if complications arise.
Residential Treatment
Residential treatment, also known as inpatient rehabilitation, provides a structured, live-in environment where individuals receive round-the-clock care. This level of care is appropriate for people with severe addiction, those who have relapsed after lower levels of care, or individuals who lack a stable home environment. Residential programs typically include daily therapy sessions, group therapy, medical oversight, and life skills development.
Partial Hospitalization Program (PHP)
A partial hospitalization program offers intensive treatment during the day while allowing the individual to return home or to a sober living environment in the evening. PHP typically involves several hours of programming per day, multiple days per week, and includes individual therapy, group therapy, medication management, and psychiatric support.
Intensive Outpatient Program (IOP)
An intensive outpatient program provides a step down from PHP, offering structured therapy and support while allowing individuals to maintain work, school, or family responsibilities. IOP typically meets several times per week for a few hours per session and includes group therapy, individual therapy, and relapse prevention planning.
Outpatient Counseling
Outpatient drug and alcohol treatment is the least restrictive level of care and is often used as a long-term maintenance option after completing a more intensive program. Outpatient counseling may include weekly or biweekly individual therapy, periodic group therapy, and ongoing medication management.

Support Systems and Recovery Resources
Recovery from fentanyl addiction does not end when a treatment program is completed. Building a strong, sustained support system is one of the most important factors in maintaining sobriety over the long term.
Professional and Peer Support
Individual therapy provides ongoing, one-on-one support for processing the psychological dimensions of addiction and addressing co-occurring mental health challenges such as depression, anxiety, or trauma.
Group therapy connects individuals with others who share similar experiences, providing accountability, encouragement, and a sense of community.
Peer support specialists are individuals who have their own lived experience with addiction and recovery. They serve as mentors and advocates, helping others navigate the treatment system and stay engaged in recovery.
Recovery coaches provide practical, goal-oriented support, helping individuals build the skills and routines needed to sustain recovery in everyday life.
Harm Reduction
Harm reduction strategies play a vital role in keeping people alive and connected to care, even when they are not yet ready for or engaged in formal treatment. Naloxone (Narcan) is a life-saving opioid antagonist that can reverse an overdose in progress and is a cornerstone of overdose prevention efforts. Carrying naloxone and knowing how to use it can mean the difference between life and death for someone exposed to fentanyl. Fentanyl test strips, syringe service programs, and safe use education are additional harm reduction tools that reduce risk and build trust with individuals who may eventually seek treatment.
SAMHSA Resources
If you are unsure where to begin, SAMHSA’s National Helpline (1-800-662-4357) is a free, confidential, 24/7 information and referral service for individuals and families facing substance use disorders. SAMHSA’s treatment locator and the Buprenorphine Providers Locator (SAMHSA) can help you find treatment facilities and qualified prescribers in your area.

Special Considerations in Treatment
Pregnant and Postpartum Women
Opioid use disorder during pregnancy requires specialized care. Methadone maintenance treatment and buprenorphine are recommended for pregnant and postpartum women, as medically supervised treatment is safer for both the mother and the baby than unsupervised withdrawal. Treatment programs that serve this population provide coordinated prenatal care, addiction medicine, and postpartum support.
Co-Occurring Mental Health Conditions
Many individuals with opioid use disorders also experience co-occurring mental health challenges such as depression, anxiety, PTSD, or other conditions. Effective treatment addresses both the substance use disorder and any mental health conditions simultaneously through an integrated treatment plan, which may include psychiatric medication, therapy, and ongoing monitoring.
Side Effects of Medications
All medications for opioid use disorder can produce side effects. Common side effects vary by medication but may include constipation, nausea, drowsiness, headache, and sweating. Your treatment team will monitor for side effects and adjust your treatment plan accordingly. It is important to discuss any concerns about medication with your provider rather than stopping treatment on your own.
Accessing Fentanyl Addiction Treatment in NY
Reducing Stigma Around Treatment
One of the biggest barriers to seeking help is stigma. Opioid use disorder is a medical condition, not a moral failing. Reducing stigma — in communities, in healthcare settings, and within families — is essential to ensuring that people feel empowered to ask for help. CDC campaigns and public health initiatives continue to work toward changing the narrative around addiction and treatment, including efforts like the Rx Awareness campaign that shares real stories of people affected by prescription opioids.
How to Get Started
Taking the first step toward treatment can feel overwhelming, but the process is simpler than many people expect:
- Reach out. Contact a treatment provider, your primary care doctor, or call SAMHSA’s National Helpline at 1-800-662-4357 for guidance.
- Complete an assessment. A clinical assessment evaluates the severity of your substance use, your physical and mental health, and your social situation to determine the most appropriate level of care.
- Understand your insurance options. Most health insurance plans, including Medicaid and Medicare, are required to cover substance use disorder treatment. Many treatment centers have admissions staff who can verify your benefits and help you understand your coverage.
- Begin treatment. Whether that means starting medication in an outpatient setting, entering a residential program, or beginning with detox, the most important thing is to start.
You do not have to wait for a crisis to seek help. Treatment is most effective when accessed early, but recovery is possible at any stage.

Find Fentanyl Addiction Treatment in NY at Mid Hudson Addiction Recovery
At Mid Hudson Addiction Recovery, we provide compassionate support and evidence-based treatment for individuals struggling with fentanyl and other opioid addictions. Our network of New York treatment centers offers the full continuum of care, from medically supervised detox through outpatient counseling and ongoing recovery support.
Every treatment plan is individualized. We take the time to understand your unique situation — your history, your goals, your challenges — and build a road to recovery that reflects who you are and what you need. Whether you need residential treatment, an intensive outpatient program, medication management, or a combination of services, we are here to help.
You do not have to face this alone, and you do not have to travel out of state to get the care you deserve. Talk to our team today to take the first step toward reclaiming your life.
